Kneecap Joint Dislocation
If you have further questions about kneecap joint dislocation then please feel free to contact us
here.
Alternatively you can book an appointment to see us below.
The patellofemoral joint is one of the three compartments in the knee. It consists of an articulation between the back of the kneecap (patella) and the front of the thigh bone (femur). The main role of the kneecap is to increase the lever arm of the thigh muscles (quadriceps), making it easier to extend (straighten) the knee. The longer the lever arm, the smaller the force that is needed to extend the knee.
The kneecap is normally held firmly in place owing to the action of muscles, ligaments and the overall shape of the joint, however as a result of the alignment of the shin bone (tibia) and the thigh bone there is a natural predisposition for the kneecap to move laterally (outwards). In some patients, the kneecap joint does not form normally and this makes them more likely to develop problems with kneecap instability.
A dislocation is when two bony surfaces completely lose contact with each other. In patellar dislocation, the kneecap loses contact with the thighbone and pops out laterally. Patella dislocation may be traumatic, such as following a violent twisting injury to the knee or atraumatic without any history of trauma at all. Patients with traumatic dislocation may have an otherwise normal knee joint while patients with atraumatic dislocation may have a knee joint which has not formed normally and therefore predisposes them to patella dislocation.
What factors predispose you to patellar instability?
The most common abnormality is a shallow or absent groove on the front of the thighbone (trochlear dysplasia). Other common causes include a high kneecap (patella alta), ligament laxity, or a twist (torsion) in the shin or thighbone. There is very often a history of this problem running in the family.
When the knee dislocates it will become painful and often very swollen. There may be a feeling of instability in the knee and it may be difficult to walk. Those patients with traumatic dislocation can generally be expected to make a full recovery, although some may experience a lack of trust in the knee when they return to sports. In patients with atraumatic instability who have an underlying abnormality in their knee, further pain, swelling and instability is commonly experienced. More than half of this group of patients will experience another dislocation.
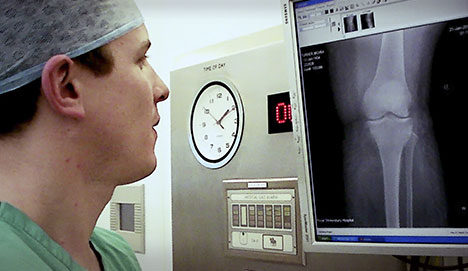
You will be asked a detailed series of questions by your surgeon. An examination will then be performed. Patellar dislocation commonly follows an identical mechanism of injury to that which leads to rupture of the anterior cruciate ligament (ACL). It is very important to exclude this injury and make the correct diagnosis. X-rays are taken to exclude any associated broken bone (fracture). An MRI scan of the knee is performed routinely to look for any evidence of the predisposing factors listed above. MRI is particularly good at looking at the soft tissues such as ligaments and cartilage which the x-rays fail to display.
Patellar dislocation is a very debilitating condition and makes physical activity such as sports very difficult indeed. It is important to stabilise the knee cap in order to prevent future arthritis in the kneecap joint.
What is the treatment?
If it is the first time your knee has dislocated, it is accepted practice to treat this conservatively (without an operation). First-line treatment consists of RICE (Rest, Ice Compression and Elevation). In addition, painkillers and anti-inflammatory medication are advisable. You will be referred for physiotherapy to help strengthen the quadriceps muscles and regain full range of motion. In the past, patients were treated in plaster for 6 weeks with the knee held out straight, however we now know this is a bad idea because the knee becomes very stiff indeed and the thigh muscles waste away. If patellar dislocation becomes a recurrent problem and conservative treatment has failed, surgery will be offered. There are three operations which are commonly used to treat patellar instability.
Medial patellofemoral ligament reconstruction
The medial patellofemoral ligament (MPFL) runs between the inner side of the kneecap and the inner side of the thigh bone. It has been shown to provide 60% of the stability of the kneecap joint. It is torn in all cases of true patellar dislocation. The operation uses one of your hamstring tendons to reconstruct this ligament. A tunnel is drilled across your kneecap and also on the inner side of your thigh bone. The tendon is passed through these tunnels and fixed with a special device called an endobutton® in the kneecap and a screw in the thigh bone. This is a very successful operation if used for the right indication.
Tibial Tubercle Osteotomy
If you have a high kneecap (patella alta) or you have a twist in the femur or shin bone it may be appropriate to perform an osteotomy (bone cut) at the tibial tubercle. The tibial tubercle is the prominent piece of bone felt on the front of the knee where the kneecap tendon (patellar tendon) inserts. Once the tibial tubercle is cut, it is repositioned to correct the underlying abnormality and fixed in place with two screws. It normally takes 6-8 weeks for this bone cut to heal after which normal weight bearing without crutches can resume.
Trochleoplasty
This operation is undertaken in only a handful of centres in the UK. It is used in patients whose knees have developed abnormally such that the front of their thigh bone is dome-shaped or has a large bump rather than a groove. Trochleoplasty involves creating a new groove in the thigh bone for the kneecap to sit in.